Search Blog
Your Blog Roll
Signup to get the latest News & Resources
Connect with us
Posted by Peter Hunt in General on August 26th, 2019

Whether you’re a Pilates devotee or brand new to the practice, you’ll gain a lot from Pilates classes at The Alignment Studio. With two different styles on offer—Reformer Pilates and Studio Pilates—you’ll improve your flexibility, posture, coordination and range of motion. Injured? Try our Clinical Rehab classes. Designed and run by physios, these private or semi-private therapeutic sessions draw upon Pilates based exercises to ensure a full and speedy recovery.
Read on to learn more about Pilates at The Alignment Studio, and to find the class that’s right for you. (We have a maximum of 6 per class, so you’ll need to move fast to secure your place—call us on 9650 2220, book online or via The Alignment Studio app!)
For a fun, fast-paced Pilates class in Melbourne CBD, look no further than The Alignment Studio’s Express Reformer classes. Offering a top-to-toe workout in 45 minutes, our Express Reformer classes are a great way to stretch (and sweat) it out after a long day in the office. Helping to correct your posture and alignment and improve your balance, strength, core stability and coordination, a single session will help you stand taller!
What to expect?
Taken by qualified Pilates instructors, Express Reformer Pilates classes at The Alignment Studio are conducted on, and around, Pilates Reformers. The Reformer itself is a highly versatile structure with a rolling carriage, springs, straps and footbar that allows you to safely train and challenge different areas of the body. Throughout the class, you can expect to lie, sit, stand and kneel on the Reformer, perform movements with your legs and arms in straps, and utilise equipment including Pilates boxes, magic circles and hand weights.
By changing your springs when instructed, you’ll increase or decrease resistance for a different type of challenge. While heavier springs will help strengthen and tone, lighter springs will engage your stabilising muscles as you attempt to hold the carriage in place.
Breathwork is a core Pilates principle, and you’ll learn how to utilise your breath to deepen into each stretch and increase your flexibility and range of motion. You’ll also experience a new level of body awareness.
At The Alignment Studio, we intentionally keep our Reformer Pilates classes small (6 people or under) to ensure a safe practice. While students follow the same sequence of exercises, our small class sizes allow instructors to correct individual posture and technique as required. Adjustments can also be made for different abilities, injuries and how each student is feeling/ presenting on the day.
Are Reformer Pilates classes for me?
No matter your age, sex or fitness level, Reformer Pilates is a safe and incredibly inclusive movement practice that enhances mobility and mind-body connectedness. The Alignment Studio’s Reformer Pilates program caters to beginner Pilates students through to experienced practitioners and athletes.
You’ll benefit from our Express Reformer classes if you are:
• New to Pilates
• Experienced with Reformer, Studio or Mat Pilates
• Recovering from injury (Clinical Rehab or Studio Pilates may be more suitable, please ask our friendly team)
• Fit, starting from scratch, or somewhere in between!
• Sedentary or ultra-active
• Pre or postnatal (with clearance from your doctor)
• Experiencing back pain or postural issues
• Wanting to improve core strength and stability
• Looking to improve flexibility and mobility
• A desk-bound office worker
• Seeking a new fitness challenge
• Wanting to enhance your strength, endurance and sporting performance
• Looking for a comprehensive, full-body workout in under an hour!
Utilising a range of Pilates equipment such as Reformers, Trapeze Tables, Wunda Chairs and Spine Correctors, Studio Pilates at The Alignment Studio is a highly personalised practice. Private or semi-private, with a maximum of 3 people per class, each 50-minute session will include exercises tailored to your unique physical condition and goals. For instance, if you have an injury, your Studio Pilates program might be more rehabilitative than fitness-based.
What to expect?
Studio Pilates sessions are taken by highly skilled and qualified Pilates instructors. You will be given your own goal-oriented program, and can expect plenty of one-on-one attention, even in a small-group class. You’ll also reap the benefits of using a full range of Pilates equipment.
Is Studio Pilates for me?
If you are new to Pilates, rehabbing an injury, or want to improve specific aspects of your physical performance, consider giving Studio Pilates a go. You will benefit from personalised attention and a program that is fully tailored to you and your unique goals. You’ll enjoy moving at your own pace and having the focused support and attention of a skilled instructor.
Studio Pilates is often recommended following completion of a Clinical Rehab program.
Clinical Rehab classes are not pure Pilates classes; they are active physiotherapy sessions that draw on a range of Pilates practices to enhance your recovery. Ideal for those with chronic and acute injuries or biomechanical dysfunction, our Clinical Rehab classes are therapeutic, evidence-based sessions taken by physiotherapists. Depending on your cover, these 45-minute sessions may be claimable on private health.
What to expect?
Designed to support your unique rehabilitation journey, Clinical Rehab classes are entirely personalised. You will be thoroughly assessed by a physiotherapist and given your own program prior to starting private, duet or small-group (maximum 4 people) classes. Your assessment may utilise real-time ultrasound to identify and correct muscle activation.
Classes include a mix of treatment and movement, and may incorporate Pilates equipment such as foam rollers, Pilates rings, pulleys, Reformers, resistance bands, light weights, kettlebells and more.
Our Clinical Rehab classes empower you to take an active part in your recovery. They can be very beneficial in the case of:
• An acute or chronic injury
• Neck or back pain
• Rotator cuff and shoulder issues
• Hip, knee or ankle pain
• Postural problems
• Balance and coordination issues
• Limited mobility
• Women’s and maternal health (pre and postnatal)
• Chronic disease
• Neurological conditions
Bookings are now available for our Clinical Rehab and Pilates classes in Melbourne CBD. Call us on 9650 2220 for more information, book classes online or download The Alignment Studio app.
Posted by Peter Hunt in General on July 9th, 2019

If we’ve seemed distracted the past few months, it’s because we’ve been working on a little something that’s actually kind of, well, big. Now the paint is almost dry we can finally reveal our secret—next month we’re opening a shiny new studio/ clinic that’s set to be THE go-to destination for physiotherapy, massage, yoga and Pilates in Melbourne CBD!
A tranquil space to realign your body, mind and spirit, The Alignment Studio will introduce a refreshingly integrated clinic model that combines the best of health, fitness and wellbeing services under one convenient roof. From physiotherapy to Pilates, remedial massage, podiatry, clinical rehabilitation, women’s and men’s health physiotherapy, yoga and nutrition coaching, all your wellness needs will be catered for. All within one Collins Place location. How’s that for convenience?
At The Alignment Studio, we believe regular movement is vital to nourish the body and mind, and the antidote to our increasingly sedentary, desk-bound, device-addicted lives. We believe we are best equipped to achieve our goals when our bodies and minds are aligned. We also strongly believe in the power of collaboration.
We’ve therefore set about creating a stress-free zone where you can unplug, unwind and recharge, free from distractions, as our team works together to restore your mobility and bring your body and mind back into balance. The Alignment Studio will enable those with pain, injury or illness, as well as the super-fit and athletic, to safely enjoy the benefits of Pilates and yoga as they move towards recovery.
Our commitment to your wellbeing means we’ll not only alleviate your symptoms, but dig deeper to uncover the root cause of your pain or discomfort. We’ll also empower you with the self-management tools and knowledge to invest in yourself, so you can enjoy pain-free, uninhibited movement, and live a full and balanced life!
In our sleek, cutting-edge Melbourne CBD clinic and fitness studio you’ll have access to the following services:
• Physiotherapy
• Remedial Massage
• Reformer Pilates
• Clinical Rehab Classes (active physiotherapy sessions that include Pilates-based exercise/equipment)
• Yoga
• Podiatry
• Integrative Nutrition & Health Coaching
• Women’s Health Physiotherapy
• Men’s Health Physiotherapy
We can also create a bespoke wellness package, class or demonstration for your team.
Good question! Collins Place Physio will no longer operate from its current premises, but the entire team will now be found at The Alignment Studio. So, rest assured you’ll still have access to your favourite physio or massage therapist. Plus a crop of fresh faces we hope you’ll get to know as you try our additional services!
The Alignment Studio will be located at Shop 19, Collins Place (45 Collins Street). While the exact opening date is TBC, building is well and truly underway, and we can confirm an early-to-mid August unveiling. STAY TUNED!
Posted by Peter Hunt in General on June 12th, 2019

Maintaining healthy, happy feet is extremely important—after all, you’re on them for much of the day! Without foot comfort, your mobility becomes increasingly restricted, and this restricted mobility can in turn have serious implications for your general health. Because we’re committed to helping you optimise your health, from top to toe, Collins Place Physio’s resident podiatrist Louise Anderson has put together a handy list of nine sure-fire signs you should see a podiatrist. If any sound familiar, it’s time to book an appointment and take the first steps towards improving your foot health, today.
Sore toes and/or soles of feet can occur because shoes are too tight and may be too high in the heel. This places pressure on different parts of the foot, resulting in excessive hard skin and the development of corns. These can be removed fairly simply, and different shoes might be an additional solution recommended by your podiatrist.
Cracked heels can simply occur as the result of very dry skin. However, in certain people, the skin overreacts to pressure and dryness and produces excess keratin, resulting in callouses and cracks. Treatment and a daily management program recommended by your podiatrist can help with both concerns.
Thick nails, fungal, ingrown, and curly nails can cause great discomfort, even in well-fitting shoes. Thankfully, any number of nail problems can be dealt with with proper podiatry care.
Papillomas (a viral skin infection, known as verrucas) are a frequent issue for people who go barefoot into swimming pools, gyms and public bathrooms. While wearing flip-flops is a good preventative measure, if you already have papillomas, a podiatrist should be your first port of call.
Itchy feet? Interdigital tinea and general fungal infections are very common—often picked up from other people, and sometimes related to poor hygiene. A podiatrist will be able to recommend the right course to resolve your fungal foot problems.
Pain throughout the body, for example in the hips, ankles, knees, shins or lower back, can often begin in the last place you’d expect—the feet. For this reason, podiatrists and physiotherapists will often work together to improve a patient’s bodily alignment and resolve pain. Have you ever checked the soles of your shoes to see where the wear occurs? If the wear is uneven, you may need correction. Do you feel that your feet are rolling in? The realignment of your feet with corrective orthotics can remove discomfort in many areas of your body.
These are signs of soft tissue inflammation (often plantar fasciitis) caused by poor biomechanics of the feet. With a regime of exercise (stretches) and orthotics, this debilitating condition can be overcome.
A podiatrist has many cushioning and padding materials, including soft insoles, which can assist in protecting joints in people of all ages with all types of arthritis that affect the lower limbs.
Podiatrists undergo many years of training to become very skilful in fine motor skills. They are therefore the only practitioners that should be allowed to tend to the feet of those with compromised immune systems or poor circulation. A podiatrist is an integral part of any diabetic’s healthcare team.
If you are experiencing any of the above concerns, call Collins Place Physio today on 9650 2220 to discuss whether a podiatry or physiotherapy appointment may be required.
Posted by Peter Hunt in General on June 10th, 2019

Looking for a skilled podiatrist in Melbourne CBD? You now need to look no further than Collins Place Physio. In addition to our physiotherapy and remedial massage services, we’ve added podiatry to the mix—welcoming the lovely Louise Anderson to the CPP family. With over 30 years’ experience in podiatry in Melbourne and the UK, Louise is equipped to diagnose, treat and help prevent conditions of the foot and lower limb.
Get to know a bit about Louise, and make her your first port of call if you’re suffering from foot pain, circulatory problems, or nail and skin conditions.
My favourite part of the job is helping to relieve someone’s pain or discomfort—seeing a patient’s relief as they put their shoes on post treatment!
Running a very successful Podiatry clinic in Melbourne CBD for over 20 years. I also been fortunate to work with at-risk patients in both Hammersmith Hospital in London and Western General Hospital in Footscray.
My special interests are the treatment of ingrown/involuted toe nails, removal of corns, and treatment of papillomas. Also casting for custom-made orthotics.
Diabetics, patients with poorly fitting footwear, and patients who have an over-production of callus (hyperkeratosis).
Choosing the right footwear!
Can I have two? Wear the right footwear, and stop ‘self-treating’ your ingrown/involuted toe nails.
Yes! I will often refer to physios when I require a biomechanical second opinion. I also receive referrals from physios as a lot of referred pain, such as back or neck pain, can in fact be traced back to foot problems, such as flat feet.
I would be working in conservation of the environment, assisting with rescue horses, riding more horses, and helping older ladies to live healthy lifestyles.
Every day I try to eat fruit and a salad, exercise, remember that the glass is half full and appreciate all the good in my life. I also spend time playing with our dogs and horse, do yoga once a week, try to get a good night’s sleep, and have a good laugh.
To book your podiatry appointment with Louise, call us on 9650 2220.
Posted by Peter Hunt in General on May 29th, 2019

A strong immune system helps keep you healthy, so there’s no better time to bolster yours than during cold and flu season. According to Nutritional Therapist Tara Doherty (soon to join the CPP team!), if you’re looking for ways to prevent winter lurgies (and who isn’t?!), it’s time to hit the green grocer’s! Here, she’s started your weekly shopping list with eight fabulous immune boosting foods for winter. Read on to discover their cold-and-flu-fighting super powers, then make sure you add them to your trolley.
Most people rush out to buy Vitamin C after they’ve caught a cold. However, as your body doesn’t produce or store Vitamin C, you actually need a daily dose to maintain health. This is because Vitamin C helps build up your immune system and is thought to increase the production of white blood cells, which are key to fighting infections. Delicious citrus fruits to munch on include grapefruit, oranges, mandarins, lemons and limes. Eat the whole fruit or add a squeeze of lemon or lime to your food. Yum!
These sweet, crunchy and versatile fruits (yes, fruits) pack a powerful dose of Vitamin C, containing twice as much as citrus. They are also a rich source of beta carotene and can help optimise eye and skin health. Best eaten raw to preserve the nutrient content, capsicum is perfect for adding crunch and colour to your salad. Or try serving in sticks, alongside your favourite dip.
One of the most nutritious foods on the planet, broccoli is packed with vitamins and minerals, including Vitamins A, C and E, as well as many antioxidants. To get the best nutritional bang for your buck, serve raw (eg. as part of a salad), or very lightly steamed. Broccoli sprouts are also nutrient-dense and easy to grow at home.
Almonds contain valuable Vitamin E – essential to a healthy immune system. A fat-soluble vitamin, Vitamin E requires the presence of fats to be absorbed by the body. This makes almonds the perfect delivery vehicle as they are both high in Vitamin E and healthy fats. A handful of almonds makes the perfect portable, healthy snack, so stash some in your desk drawer, car, or gym bag.
Regularly eating garlic may help prevent the common cold or the flu, as it has immune-boosting properties stemming from a heavy concentration of sulfur-containing compounds such as allicin. Prior to cooking garlic, allow it to stand for 10 minutes after crushing or slicing to increase the allicin content. Two to three cloves a day is an effective dose to experience the benefits.
With chronic inflammation in the body at the root of most chronic disease, ginger has an important role to play in boosting wellness. It’s valued for its anti-inflammatory as well as antioxidative properties, making it a great addition to countless winter dishes. Fresh ginger may be sliced and added to a lemon and honey tea, or grated and included in soups, curries and other comforting dishes.
Spinach increases the infection-fighting ability of our immune system, with research indicating that the flavonoids found in spinach may help prevent the common cold in otherwise healthy people. Healthiest eaten raw, spinach is also rich in antioxidants called carotenoids, as well as Vitamins C and E. Your spinach should also ideally be organic, due to high levels of pesticides used in standard farming practices.
Packed with powerful antioxidants shown to enhance immune function, green tea is the perfect health tonic all year round. A great low-caffeine alternative to coffee, it’s also a good source of L-theanine – an amino acid that may aid in the production of germ-fighting compounds. And, if you find the pure form not to your liking, there are some great infusions available. Green Tea and Pomegranate is my particular favourite.
Another great way to boost your immunity this winter? With remedial massage! Book now.
Posted by Peter Hunt in General on May 20th, 2019

As CBD physiotherapists, we see patient after patient come through our doors with poor posture, often as the result of long days spent chained to their computers. Not only do their postural problems look bad (think hunched back, rounded shoulders), they often result in tension and pain. So, because our aim at Collins Place Physio is to help you feel (and look) your best, our physios have put together this list of six of the most common signs of poor posture. Read on to discover how your posture stacks up, and to learn some tricks to help you sit, stand and walk a little taller.
Occurring in tandem, high rounded shoulders and tight pectoral muscles are signs of poor posture common among office workers. Excessive time spent sitting at a computer can lead to a tightening and shortening of the muscles in the front of the shoulders (pectorals), and a lengthening and weakening of the back muscles.
Rounded shoulders can also result from muscular imbalances that occur when too much focus is placed on developing the chest muscles at the gym, while neglecting the upper/mid back. Doing so places increased strain on the shoulder joint and can cause rotator cuff tears and impingement.
Rounded shoulders can be corrected by stretching the front of the chest and neck, while strengthening the back muscles.
A forward head carriage arises from poor postures that cause the neck to slant forwards, usually while at the computer, or when using mobile phones or tablets. Hence the coining of the term tech neck.
This forward slant of the neck places a lot more stress on the cervical spine and can create muscle imbalances as the body compensates to find efficient ways to hold the head upright. Over time, a forward head carriage can lead to degenerative changes in the neck, cause disc bulges and, potentially, nerve impingement.
Stretching the neck muscles and restoring normal range of motion as well as strengthening the back and postural muscles will help reduce the symptoms of tech neck. With its focus on posture and movements that stretch, strengthen and stabilise, Pilates is perfect for long-term management. In the office, improving the ergonomics of your workstation, using a standing desk, and moving regularly will all help to correct a forward head carriage.
A hunched back, aka thoracic kyphosis, is another result of poor posture, and is most common in adolescents and young adults. It also often occurs alongside a forward head carriage and rounded shoulders in office workers, in a condition known as Upper Crossed Syndrome.
Another cause of kyphosis is Scheuermann’s disease, which is characterised by abnormal growth of the thoracic spine. Here the thoracic spine starts to lose mobility and become rounded, giving a hunchback appearance.
Postural kyphosis is corrected easily by standing up straight and maintaining an upright posture, alongside ergonomic improvements, while the treatment for Scheuermann’s disease involves physiotherapy and a stretching/mobility program. Bracing may also be needed if the person is still growing.
Recurring headaches are quite common among office workers with poor postural habits. A forward head carriage puts the joints and discs of the neck under a lot of strain as they struggle to support the weight of the head. The muscles of the neck are overworked in this position and it creates a lot of tension where they attach into the back of the skull. This in turn creates tension headaches. (However, they can also be triggered by stress and grinding teeth.)
Physiotherapy assessment is needed to assess the neck’s mobility and strength. Massage, dry needling and joint mobilisation will help to relieve the symptoms. A stretching and strengthening program in conjunction with an ergonomic assessment will help prevent recurrent problems.
Excessive sitting or a predominantly desk-bound job can cause tightness in the hip flexors, which run from the lower back into the front of the hip. Tight hip flexors result in the pelvis rotating forward. This can cause an increased curvature of the both the lower and upper back, which can result in pain.
The pelvis should sit in a relatively neutral position and be able to tilt backwards and forwards without any limitation or pain. General hip strengthening, especially through the glutes, as well as core strengthening can help. It is also important to break up the length of time spent sitting.
Poor posture leads to muscular imbalances and can result in pain, particularly throughout the upper body. For instance, a forward head carriage increases the workload through the neck and upper back muscles to hold the ‘increased’ weight of the head against gravity. Over time, this causes stiffness in joints and strain through the neck and upper back muscles, resulting in pain.
Break up the length of time you spend sitting, do neck and upper back stretches throughout the day, and talk to your physiotherapist about strengthening exercises to help you maintain good posture. Try to be mindful of your posture and correct often, ensuring there is a gentle curve through your neck, upper back and lower back so that your head sits directly on top of your shoulders and trunk. (Head here for postural tips when sitting and standing.)
For improved posture and reduced pain, book a Postural Analysis at Collins Place Physio by calling 9650 2220 today.
Image Source
Posted by Peter Hunt in General on May 1st, 2019

A painful condition that affects shoulder and arm movement and often causes sleep disturbance, biceps tendonitis arises when there is inflammation to the long-head bicep tendon. Common in sports and professions that involve repetitive overhead activity, this overuse injury is rarely seen in isolation. In other words, it typically exists alongside other pathologies such as rotator cuff injuries, shoulder instability, labral (shoulder fibrocartilage) tears and arthritis. Read on to discover all you need to know about biceps tendonitis, its causes, and its treatment.
Situated in the front of the upper arm between the shoulder and elbow, the biceps muscle is made up of a short head and a long head. The short head attaches to the top anterior portion of the shoulder. The long head passes through a groove at the front of the shoulder, through the shoulder joint and attaches at the top of the shoulder, making it more susceptible to inflammation and injury.
Biceps tendonitis is often present in conjunction with injuries to the rotator cuff (muscles on the back and top of the shoulder that provide stability to the shoulder joint) and/or shoulder instability because the pain, weakness and poor biomechanics in the overall shoulder function places excessive load on the biceps.
Those with biceps tendonitis will experience pain in the front of the shoulder, especially when lifting or performing overhead movements such as pulling on a jumper or putting on a jacket. There will be pain and/or weakness with shoulder flexion, ie. when lifting the arm forward and above the head. Other symptoms may include pain radiating to the elbow, pain and/or weakness when bending the elbow, pain on reaching into the back seat of the car and a clicking noise accompanying shoulder movement in the affected arm. Patients with biceps tendonitis typically also complain of pain when sleeping on the affected shoulder.
Biceps tendonitis is most often brought about by repetitive overhead actions. For instance, it is regularly seen in athletes involved in sports that require overhead activities, such as baseball (pitching), tennis (serving), and swimming. Those in jobs that require overhead activity and lifting (eg. painters, builders) are also at risk. In some instances, biceps tendonitis is brought about by trauma, while tendinosis – chronic, non-inflamed tendon discomfort due to degeneration – can be a problem for the older population.
Your physio will first take a thorough history of your injury, assess the range, strength and function of the neck, shoulder and thoracic spine to rule out other potential pathologies. Further investigation may be required in the form of an ultrasound or MRI.
If there is inflammation to the tendon (tendonitis), the first stages of treatment will typically include anti-inflammatories, ice and rest. Patients with acute biceps tendonitis – as well as the chronic, non-inflamed condition, tendinosis – will need to embark on a strengthening program.
To rehabilitate the area and prevent biceps tendonitis from recurring, it is important to strengthen the shoulder muscles and scapula, and improve posture and neck and thoracic (upper back) flexibility. Your physiotherapist will provide you with suitable exercises, and educate you on how to improve your lifting/overhead technique.
If you feel like you may be suffering from biceps tendonitis, call Collins Place Physio today on 9650 2220 to get your rehabilitation under way.
Posted by Peter Hunt in General on May 1st, 2019

While neck pain might feel like an unavoidable part of desk-job life, it needn’t be. With a few small adjustments, a little more action, and a lot less sitting, your aches and pains will occur far less often, if at all. Read on for five easy ways to reduce neck pain at work and help put an end to those nasty, neck-related headaches.
Sit-stand desks, or standing desks, allow you to quickly and easily change between seated and standing positions throughout the day. Extended time sitting at your desk is a common cause of back and neck pain at work, and a sit-stand desk can help reduce muscle tightness, tension and associated pain. Try to stand for one to two hours before sitting for 45 minutes, then returning to standing – aim to stand for more than half of the day.
With prolonged sedentary time proven to increase your risk of obesity, cardiovascular and other disease, a sit-stand desk is an investment in your wellbeing for today and into the future!
Any HR department knows the importance of a good ergonomic set-up for a healthy and productive workforce. And, while there is no end to the ergonomic office equipment you can buy, a few simple and inexpensive adjustments can also improve your workstation set-up and reduce neck pain.
Start by looking at your computer – your eyes should be in line with the top half or third of the monitor when looking straight ahead. If not, adjust your screen (and/or seat) accordingly. If you’re using a laptop, consider using an external monitor or a laptop stand (plus external keyboard) to ensure the correct eye height. In a pinch, a stack of magazines or books can also do the trick.
Adjust your seat height so that your feet are flat on the ground, with a 90-degree angle at the hips. Knees can be slightly lower, but avoid a seated position where the knees are higher as this can put pressure on the hips.
Ensure your forearms are supported on your desk (at last half the forearm should be on the desk) and that your elbows are at desk height when they are bent at 90 degrees. This applies whether you are seated or standing. (If you are not sure where to start, ask a friendly team member about Collins Place Physio’s ergonomic assessments.)
Try to do these three simple stretches in the morning, at lunchtime, and in the afternoon for reduced tension and pain in the upper back and neck.
Upper trapezius stretch – in a seated position hold onto your chair seat with your right hand. Take your left ear down towards your left shoulder, then tilt the chin slightly to the right. With your left hand, gently push the side of the head downward to the left. You should feel a stretch in the right side of the neck and the top of the shoulder. Hold for 20 seconds and repeat 2-3 times. Repeat on the other side.
Levator scapulae stretch – hold your chair seat with your right hand. Take your chin towards your chest, turn your head gently to the left, then bend your head downwards taking your left ear towards your left hip pocket, using your left hand to apply downwards pressure to the back of your head until you feel a gentle stretch above your right shoulder blade. Hold for 20 seconds and repeat 2-3 times. Repeat on the other side.
Anterior cervicals – pull your collar bones down, then gently bend your neck backwards. Hold for 20 seconds, and repeat 2-3 times.
If you find you regularly suffer from neck pain and headaches, it may pay to have an eye check. Straining towards your monitor with a forward head position is frequently a cause of neck pain and cervicogenic headaches. And constant squinting and eye strain certainly won’t help, either!
If you don’t have the luxury of a sit-stand desk, make sure you still get on your feet every half hour. Not only will moving about help relieve neck and back pain and tension, it will boost your energy levels and give you a chance to connect with colleagues face-to-face. Sunny day? Instead of sitting in the conference room for that weekly WIP, suggest a walking meeting in the park.
If you are suffering from neck pain or headaches, give our friendly Collins Place Physio team a call today on 9650 2220.
Posted by Peter Hunt in General on April 2nd, 2019

As physios, we’re big believers that the more you move, the longer you live. Yet, while we’ll happily espouse the benefits of participating in sport and fitness activities for both the body and the mind, we’re also witness to A LOT of sports injuries. Because it’s our aim at Collins Place Physio to help you stay in the game, resident sports nut Conor has outlined four of the most common sports injuries, plus some useful tips for prevention. Play on!
Ankle sprains happen to people of all ages. They occur when you ‘roll your ankle’, which over-stretches the ligaments.
Symptoms
Symptoms of an ankle sprain include acute pain, swelling and bruising, as well as difficulty weight bearing/walking. The pain usually starts to subside after the first 3 to 4 days.
Causes
A sprain occurs when the ankle is suddenly twisted/rolled and forced beyond its normal range of motion, stretching or tearing the ligaments. This can occur when landing awkwardly, stepping on another player’s foot, or getting your foot caught in the ground when turning. Ankle sprains are common in all sports and activities that involve a lot of jumping, turning, and sudden changes of direction.
Prevention
In general, it is important to warm up properly and wear supportive footwear when exercising. Incorporating balance and plyometric exercises into your gym routine can also help.
Treatment
For the first 72 hours, follow the RICE (rest, ice, compression, elevation) protocol. In severe cases an x-ray or MRI may be recommended to rule out a fracture or serious injury to the surrounding ligaments and tendons and joint cartilage. Crutches may help for the first week, or a moon boot/brace/taping may be recommended to allow the ligaments to heal.
After the acute pain has eased, your physiotherapist will start you on a rehabilitation program to strengthen all the stabilising muscles and ligaments. The most important thing after an ankle sprain is to complete this rehabilitation to strengthen the surrounding musculature properly and return your proprioceptive or balance ability. Your physio will run you through sport specific exercises, i.e running, turning, jumping and landing exercises, to help prevent recurrent problems.
In the case of an ankle sprain, it can often take up to 6 weeks before a return to sport.
The rotator cuff is a group of four muscles and their tendons that arise from the shoulder blade and attach to the head of the humerus (upper arm), forming a cuff. The rotator cuff centres the humeral head in the shallow socket and provides strength and stability during motion of the shoulder joint. It also helps you to abduct (raise arm to the side), internally rotate and externally rotate the shoulder.
Symptoms
Rotator cuff injuries usually start with a nagging ache in the shoulder when lifting/reaching overhead, dressing, or lying on the shoulder at night. This develops into pain and weakness with repetitive use, or when lifting the arm overhead.
Causes
This common sports injury is mainly due to a trauma to the shoulder, or an overuse injury caused by repetitive overhead sports like tennis, volleyball, pitching etc.
Prevention
As the shoulder joint is so mobile, it depends on the strength of the rotator cuff muscles and tendons for stability. To prevent injuries to the shoulder it is important to strengthen the rotator cuff as well as the bigger muscles around the joint. Rotator cuff exercises should be incorporated into all gym programs that involve upper body strengthening. You also need to strengthen the muscles that stabilise the scapula as this provides the base for all shoulder movements. If one of these muscles is weak, it will place more stress on the rotator cuff tendons at the front of the shoulder.
Thoracic (upper back) mobility is also essential in preventing shoulder injuries. Poor mobility in the thoracic spine will cause a person to have reduced thoracic extension and rounded shoulders. This places a lot more load on the rotator cuff tendons and can increase the risk of injury.
Treatment
Rehabilitation involves strengthening the rotator cuff, the muscles that stabilise the scapula, and working on general mobility. Partial thickness tears will usually heal themselves with rest and the appropriate rotator cuff strengthening program. Full thickness tears may need to be surgically repaired if the person is returning to a high level of sport/activity. Older patients can return to normal function through conservative management by strengthening the remaining muscles of the rotator cuff.

Runners knee (patellofemoral pain syndrome) is a term used to describe pain in the front of the kneecap. It is usually caused by poor tracking of the kneecap due to a muscle imbalance at the hip/knee/ankle and/or poor biomechanics of the lower limb.
Symptoms
The main symptom of runner’s knee is a dull ache behind the kneecap (patella). It is usually aggravated by running but also squatting, kneeling, and going up and down stairs. Other symptoms can include swelling and grinding in the front of the knee.
Causes
It is obviously very common in running, especially long-distance running. However, runner’s knee can occur in any sport that stresses the knee joints, such as football, netball or skiing.
Prevention
Stretching and a good warm-up/warm-down will help prevent stress to the knee joint when training or playing sport. Gradually increasing running is very important when you haven’t been active for a while and are training for a 10km run/marathon.
Strengthening your hip stabilisers also helps to ensure that the knee tracks well and doesn’t collapse inwards when training. This is done through single leg exercises like lunges, step ups, and single leg bridges.
Treatment
Initial treatment consists of RICE for the first 72 hours. Taping can be very useful to unload the kneecap and ease the acute pain to allow it to settle.
Your physio will need to assess you to determine the true cause of your knee pain and you may need some hands on treatment to get you moving properly. Your physiotherapist will then give you a series of activation and strengthening exercises to work on the tracking of the patella and strengthening the muscles of the hip and knee.
The ACL is one of the main ligaments inside the knee that connects the thighbone (femur) to the shinbone (tibia).
Symptoms
Symptoms of ACL rupture include a loud popping sensation when it happens. There is severe pain and rapid swelling due to bleeding in the joint. You will also experience an inability to weight bear, and a feeling of instability on twisting movements as if your knee will ‘give way’.
Causes
ACL injuries are common in sports that require a lot of jumping, landing, and sudden changes in direction, such as soccer, netball, AFL, skiing, and basketball.
Prevention
Muscle strength and conditioning is very important in preventing ACL injury. Neuromuscular training focusing on balance, muscle firing patterns and landing technique can help to minimise the risk of injury.
Treatment
Initial treatment is RICE to help the acute symptoms settle, and an MRI to diagnose the severity of the tear. You may need a brace or crutches to stabilise your knee and allow the injury to settle.
If it is a partial thickness tear, your physiotherapist will start you on a rehabilitation program to strengthen the muscles and ligaments of the knee. The final stages of rehab will focus on sport-specific exercises like running, cutting, turning, landing etc.
If it is a large tear or complete rupture, the usual course of treatment is surgical repair. In the surgery the surgeon will remove the torn ACL and replace it with a tendon (usually hamstring). After the surgery, you are straight into a rehabilitation program with your physiotherapist to regain full range of motion, muscle strength and function.
It can take anywhere from 9 months up to 1 year to return to sport after an ACL reconstruction.
To improve your sporting performance and reduce your risk of injury, please call us on 9650 2220 to discuss our biomechanical assessment and screening services.
Posted by Peter Hunt in General on March 13th, 2019
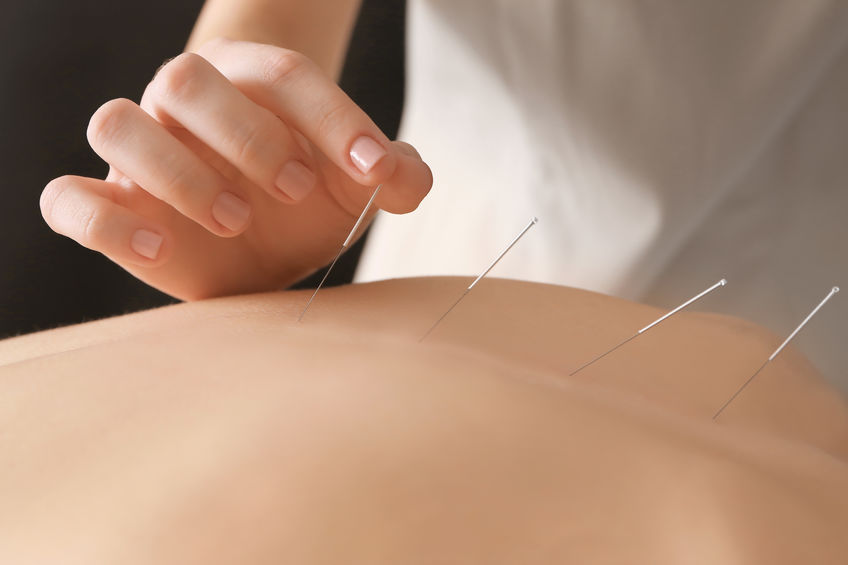
A beneficial treatment for patients presenting with acute or chronic pain, impaired mobility, or muscular tightness, dry needling is often performed alongside remedial massage or physiotherapy. But is it painful, is it hygienic, and isn’t it just the same as acupuncture? (No, yes, no.) We discuss these dry needling questions – and all the others we’re frequently asked – below. Read on to discover the important role of dry needling in fast-tracking your recovery, and to understand exactly what it is you’re in for.
In dry needling, a (fine, sanitary) needle is inserted into a myofascial trigger point to stimulate an involuntary local twitch response, which causes the muscle to release and relax. In some cases, mechanical stimulus of the needle may also be used. The successful therapeutic outcome of dry needling is to stimulate neurological sensors in the body to disrupt the contracted nature of the muscle. This can result in relief from tension, freer movement, and a reduction in pain. The technique can also cause positive local biomedical changes and result in the increase of blood flow, which in turn promotes faster recovery from your injury.
Dry needling is performed in conjunction with remedial massage or physiotherapy, and is suitable for treating most musculoskeletal conditions. These include: sprained ankles, back or neck pain, tendonitis, headache, joint pain, jaw pain, shoulder/ rotator cuff pain and impingement, bursitis, sciatica, over-use injuries, RSI, shin splits, sports injuries, ITB, tennis elbow, knee injuries, pelvic pain, plantar fasciitis, and general muscle tightness and cramping.
Dry needling is a treatment that goes deeper than manual trigger point therapy. It can also be used as an alternative to massaging an area if it is too painful. Adding dry needling to your remedial massage or physiotherapy treatment can provide faster relief from pain and muscle tightness, increase your range of motion, and speed up your recovery.
Dry needling may be slightly uncomfortable at first, but it should not be painful. You may experience a slight prick/tap when the ultra-fine needle is inserted, often followed by a twitch response. This is caused by a contraction of the muscle when the needle stimulates the myofascial trigger point/ knot in the muscle. Most patients will also experience a dull ache sensation in the area when the needle meets the trigger point.
Yes. Dry needling is performed with sterile single-use fine filament hypodermic needles (acupuncture needles).
The needles may be placed deeply or superficially, depending which area of the body is being treated. They may be left in between 5 to 7 minutes, or up to 15 minutes with the occasional manipulation or winding of the needle.
Dry needling may not be suitable for you. It is contraindicated for:
• Patients with Lymphodema
• Those with compromised immune systems (for example due to cancer, hepatitis, HIV)
• Those with vascular disease
• Diabetes
• Pregnancy
• Those with a metal allergy
• Patients on Anticoagulants (blood thinners)
The main difference between dry needling and acupuncture is that acupuncture treats to alter the flow of Qi energy based on the principles of Traditional Chinese Medicine. TCM follows the theory that Qi circulates along 12 major pathways along the body called meridians linked to a specific organ system. Dry needling, on the other hand, is based on Western anatomical and neurophysical principles relating to the trigger points – tight bands of muscle found within a muscle or muscle group.
Call us on 9650 2220 to discuss whether dry needling may be an appropriate addition to your remedial massage or physiotherapy appointment.
Posted by Peter Hunt in General on February 27th, 2019

Experiencing sudden or ongoing pain, heat or stiffness in the shoulder or hip? Bursitis could be to blame. Typically occurring in (but not limited to) these areas, this uncomfortable condition refers to inflammation of any of the body’s many bursa – small, fluid-filled sacks that provide cushioning and lubrication between a bone and joint, tendon, muscle, ligament or skin to allow smooth, pain-free motion.
When one of these sacks is inflamed, it hinders, rather than helps, movement. A swollen bursa takes up more space, resulting in increased friction and pressure, and painful, restricted movement.
If you are experiencing pain, swelling and/or heat in or around a joint, stiffness, reduced range of motion, sharp or shooting pain with movement, or pain at night that disrupts your sleep, you may have an inflamed bursa.
A common overuse injury, bursitis is often seen in individuals whose job or exercise regime involves frequent, repetitive actions. For instance, shoulder bursitis (subacromial bursitis)
may be found in a house painter, and hip bursitis (trochanteric bursitis) in a dancer. Also at risk are those who attempt to achieve too much too soon at the gym or on the sports field, without possessing adequate strength, mobility and the correct technique, or allowing enough time off for recovery.
When not brought about by frequent repetitive actions, bursitis can instead result from direct trauma, such as a car accident or a jolting fall. It is also more prevalent in those with chronic health conditions including rheumatoid arthritis.
The most common types of bursitis are subacromial – occurring between the rotator cuff tendon and acromion (bone on the tip of the shoulder), and trochanteric – occurring on the lateral surface/ outside of the hip. Inflammation to the knee, elbow and Achilles/heel bursae are also common. However, bursitis can strike anywhere a bursa is present – and there are over 100 throughout the body!
Your physiotherapist will determine your condition by assessing the joint/ muscle and surrounding areas, while taking in your medical history to rule out other potential contributing factors. Further investigations such as an ultrasound or MRI may be required.
The first steps of a bursitis treatment plan will typically include anti-inflammatories, soft tissue massage, and ice for relief. If the condition is chronic, a cortisone injection may be beneficial.
Your physiotherapist will also determine and address the causes of your bursitis for long-term and preventative management. This may involve creating a treatment plan to overcome biomechanical/muscle weakness issues with strengthening exercises and stretches, education to improve sporting technique, and lifestyle changes to reduce repetitiveness of tasks.
If you feel like you may be suffering from bursitis, call Collins Place Physio today on 9650 2220 to get your rehabilitation under way.
Posted by Peter Hunt in General on February 13th, 2019

You probably know by now how to treat an ankle sprain with the RICE method. But when else should you treat an injury with ice? And what about heat? Is it the right thing to apply for sharp lower back pain, and what about that niggling neck ache? To make sure you’re getting your temperature therapy right, read on. We’ll guide you through the ice versus heat decision, and help you recover sooner.
Ice should be used for all acute injuries and when there is inflammation. Inflammation is a natural response of the body to a trauma or injury. By constricting the blood vessels, ice helps to reduce inflammation and tissue damage. It also acts as a local anaesthetic, numbing the soft tissues and slowing down the pain messages being transmitted to the brain.
On the other hand, heat can be beneficial for general muscle aches, joint stiffness, chronic pain, and stress. Heat increases blood flow which relaxes tight muscles and relieves aching joints. A heat pack or hot water bottle is also lovely and warming on a chilly morning!
Using heat in the acute stages of an injury will increase the pain and inflammation, which can delay healing. Ice should not be used on muscle cramps/spasm as it will only cause the muscle to contract further and cause more pain. If in doubt, speak to your physio.
In some instances, yes. Alternating ice and heat has been shown to have some benefit in reducing exercise-induced muscle soreness. The ice works as an analgesic then the heat promotes blood flow to the affected area for faster recovery. Elite athletes will often use contrast water therapy (CWT), immersing themselves alternately in both cold and hot water.
The general rule for icing is ’20 minutes on and 20 minutes off’. Ice should be applied for the first 72 hours after an acute injury or trauma. It is important to make sure the ice pack is wrapped in a damp cloth (if it does not have a cover) to protect the skin from unpleasant ice burns.
Heat packs should be applied for 20 minutes up to 3-4 times per day. Single-use patches and wraps can be used continuously for up to 8 hours. If the heat pack is very warm, take care to avoid burning the skin by placing a towel between the pack and your skin.
Always avoid applying a hot or cold pack over an open would. And, if there is impaired sensation in the injured area, steer clear of both ice and heat and book an appointment with your physio.
Posted by Peter Hunt in General on January 30th, 2019

Standing desks, also known as sit-stand desks, have received a lot of attention in recent years. But are they worth the investment? In a word, yes! All the team at Collins Place Physio alternate between sitting and standing, and we recommend our office workers do too. Not convinced? Read on for the many benefits of sit-stand desks, and you’ll soon be adding one to your new year wish list!
Standing burns more calories than sitting, so switching things up and standing for periods throughout the day can help reduce your risk of weight gain. According to leading manufacturer of ergonomic solutions BakkerElkhuizen, the heart pumps around 10 times as much blood around your body if you alternate between sitting and standing, as opposed to sitting only. And you can burn approximately 145 calories in a few hours standing at your desk!
It’s not just about aesthetics either – maintaining a healthy weight plays a crucial role in avoiding the onset of type 2 diabetes and its associated complications.
Being sedentary – i.e. spending eight hours a day, five days a week sitting at your desk (!) – is akin to smoking when it comes to negative health impacts. Time and again, prolonged sedentary time has been linked to not only higher blood sugar, obesity and type 2 diabetes, but also heart disease and even some types of cancer.
According to Alpa Patel, PhD, strategic director of the American Cancer Society Cancer Prevention Study 3: “Sitting time research is still in its infancy. We are trying to understand whether it’s the total amount that you sit or how frequently you break up those bouts of sitting that are most relevant to disease risk. While we continue to learn what is driving this relationship, it’s already clear that cutting down on the time you spend sitting has good consequences for your health.”
This reduction in sitting time at work can easily be achieved with the introduction of an adjustable sit-stand desk, as well as ensuring you take plenty of active breaks. Even if that’s just walking to a colleague’s desk rather than emailing.
Sitting for extended periods can cause muscle tightness and increased tension in the lower back and even other parts of the body like the neck and upper back. For those with back pain that is aggravated by sitting, the ability to stand while at work gives significant pain relief.
Standing all day is not recommended either. As you fatigue from standing, you often start to adopt unfavourable postures, such as slouching to prop yourself up on the desk, or leaning towards one side/leg/elbow, which can lead to an increase in load and tension on that particular side.
Being able to be mobile and move from sitting to standing throughout the day helps with force/load distribution, and also helps maintain muscle length.
Proponents say the benefits of sit-stand desks extend beyond the health gains, citing higher energy levels, focus and productivity, as well as enhanced creativity. No surprise then that sit-stand desks are the go-to for tech giants Google, Apple and Facebook.
Perhaps the most compelling potential benefit of a sit-stand desk relates to your life span. Published last year, one Deakin University study of 231 desk-based workers concluded that sit-stand desks could help save 7,492 ‘health-adjusted life years’ through prevention of obesity, type 2 diabetes and heart disease.
Interested in purchasing a sit-stand desk or want to know more? Call our friendly team today on (03) 9650 2220.
Posted by Peter Hunt in General on January 3rd, 2019

Not sure if the pain or discomfort you’re experiencing is par for the course or something worth investigating? You’re not alone. To help, we’ve rounded up nine clear-cut signs you need to see a physio. And get your body back functioning at its full potential!
Headaches aren’t always a result of dehydration, eye strain, illness or stress – they are often caused by muscular tension in the neck or jaw, as well as poor posture. In many cases, your physiotherapist can assist with relieving your symptoms and assign exercises to prevent headaches from recurring. If your headaches are of a more severe nature, they will of course refer you to a medical professional.
If you’re struggling with your balance more than usual, it’s time to make an appointment with your friendly physio. There are a number of reasons your balance could be out of whack and your physiotherapist will be able to help by assessing the causes of your balance issues, then prescribing an exercise regime to restore your equilibrium.
If you’re suffering from chronic back pain or a bung shoulder, it can be a struggle to manage the recommended eight hours of shut eye. Alleviating pain will help you to sleep better, and awaken bright and refreshed, rather than grumpy and achy. Your physio will also be able to advise on the right mattress/ pillow/ sleeping position to suit your individual needs.
Recurring injury can be an indicator of inefficient movement patterns, restricted mobility, or underlying musculoskeletal issues. Your physiotherapist will be able to help correct any imbalances and provide strengthening and mobilising exercises. Ensuring those little accidents occur far less frequently!
If you frequently experience ear ache, facial pain, a clicking noise when yawning or eating, headaches, tinnitus or neck pain, you could be suffering from TMJ or jaw dysfunction. A physiotherapist with experience in this area (such as CPP’s Pete Bond) will be able to assist you in managing pain and correcting dysfunction with techniques including muscle massage, mobilisation and dry needling.
If shin splints are derailing your training plans, a trip to the physio can be very beneficial. Your physiotherapist will be able to run a full biomechanical screening, assess your technique and identify any muscle dysfunction, advise on shoe choice and orthotics, and tailor a program to improve lower limb strength, stability and mobility, and expediate your return to running.
Sharp pain in your heel, particularly during the morning, is a sign you may be suffering from plantar fasciitis. Older people, overweight individuals, pregnant women, those with high arches or arthritis, and active folk with tight calf or lower leg muscles, are more susceptible to this condition. A physiotherapist can help alleviate your symptoms with soft tissue massage and taping, equip you with beneficial stretches, and address any biomechanical issues that may be at play.
Being able to move freely is important for your sense of vitality, and mobility – like strength or fitness – is something that needs consistent work to maintain. Aside from helping you feel youthful and agile, maintaining a good range of motion will substantially reduce your risk of injury. Regardless of whether you’re loading your joints at the gym, or simply bending down to pick up a toddler.
A physiotherapist will address any issues hindering your movement and provide stretches and strategies for home, such as self-myofascial release using a foam roller or spiky ball.
This one’s a no brainer! If you are experiencing acute or ongoing bodily pain that feels muscular or joint-related, an appointment with a physiotherapist should be your first port of call.
Posted by Peter Hunt in General on December 13th, 2018

The Christmas holidays are a special time of year – a chance to kick up your heels, relax, and spend quality time with family and friends. The champagne/beer/wine’s flowing, the cricket’s on the TV, and the leftovers are seemingly endless. But for many, so too is the temptation to totally forget about good habits, and start the new year with an inevitable hangover, aches and pains, and a bit of extra padding…
While it’s fine to loosen your belt a little and relax the rules, don’t let this holiday be a complete blow out! Here’s how to easily incorporate some healthy habits into your break, and start 2019 off on the right foot.
Speaking of feet, if you live in flip flops all summer long, you might be doing yours less of a favour than you think. Regular thongs offer very little in the way of arch support, encourage pronation (inwards rolling) and put foot ligaments and joints under stress as you claw your toes to keep your thongs, well, on your feet. Regular wear can result in foot, ankle and calf pain, and conditions such as Achilles tendinopathy.
Thankfully, there is a better alternative – Archies Arch Support Thongs. Equally stylish, these physio-designed thongs are the comfiest footwear you’ll ever wear. In fact, if you bump into any of the Collins Place Physio team this break, chances are we’ll be sporting our Archies!
It might seem indulgent, but a massage can go a long way towards easing accumulating tension during the (often fraught) festive season. Christmas parties, last-minute shopping, cooking and hosting the extended family can really take their toll, and a massage can help you soldier on by boosting your immune system and easing stress.
Instead of just watching sport from your armchair, how about gathering the troops for that great Aussie tradition – a game of beach cricket? Walk off your Christmas lunch, make tennis dates with your friends, hit the gym, go for a surf or head to yoga. Now that you actually have some free time, why not use it to stay active? You’ll feel so much better for moving your body, and won’t need to start from scratch in the new year.
Taking a break from your devices is good news for both the body and mind, and allows you to be fully present when spending time with your loved ones. You don’t need to do a total blackout, but try setting limits and work to break the constant scrolling cycle. Turning off your tech two hours before bed will also ensure you sleep more soundly over the break, meaning you’ll return to work refreshed and recharged.
While we’re no grinches and think everyone should have a no-limits cheat day on December 25th, try not to let that become a cheat fortnight! Stick with the 80:20 rule (80% clean and 20% indulgent) as much as possible and you’ll start the new year feeling healthy and energised. Instead of bloated, sluggish and in dire need of a detox!
Posted by Peter Hunt in General on December 12th, 2018

Tech neck, text neck, one thing’s for sure – device-related neck pain is a modern epidemic. From smart phones to tablets, eReaders and laptops, the technology designed to enhance our lives and give us increased mobility can, ironically, hinder it. Resulting in chronic pain, reduced movement, and – if left unchecked – costly rehabilitation bills.
Caused by an over reliance on mobile devices, tech neck is certainly an increasingly common complaint in our Melbourne CBD physiotherapy clinic. Thankfully, however, it can largely be prevented, without the need to go cold turkey.
They’re lighter and more portable than ever before, so how exactly are our smart phones and laptop computers doing us damage? The answer lies in the posture we assume when reading, typing or texting.
Prolonged flexion of the neck (looking down) encourages a forward shoulder posture which puts the neck further forward, out of the base of support. This means the neck and shoulder muscles need to work harder to hold your head up against gravity. Over time, this overuse can lead to fatigue and chronic neck pain.
If you are experiencing the following, take notice:
Nobody says you have to turn into a luddite, but limiting your mindless scrolling has numerous benefits for your physical, not to mention mental, wellbeing. Try using an app to track your screen time, and set yourself strict daily limits for social media.
Instead of sending dozens of text messages to the same person, save your neck (and your thumb from RSI!) and consider engaging in the declining art of phone conversation. Popping your phone on speaker or pairing with Bluetooth headphones when out and about will help prevent any crick in the neck caused by lengthy chats.
In the office, instead of emailing that colleague three seats away, drop by their desk and discuss the project in person. And, if you work from home, try to avoid falling into bad habits, like working from your couch or kitchen table. A good ergonomic home office setup is vital for productivity as well as your wellbeing. (If you are unsure where to start, contact us for an at-home ergonomic assessment.)
Regularly read from a tablet or Kindle in bed, or on the bus/train/tram? This could be the underlying cause of your tech neck. To avoid this, sit with your back slightly reclined and prop up your eReader with pillows so that it sits at eye level. This helps to reduce the workload on your neck and shoulder muscles.
If you are experiencing signs of tech neck, your first course of action (after reducing your screen time) is to book a physiotherapy assessment. Treatment will typically include a combination of soft tissue massage, joint mobilisation and, in some cases, taping. Consider booking a professional ergonomic assessment of your workstation, and seek postural advice.
Your physiotherapist may also prescribe a strengthening program for your back and postural muscles, and the smaller muscles that help stabilise the neck. Working on your posture will be very beneficial and, in the longer term, Pilates may help to prevent recurrence.
Posted by Peter Hunt in General on November 22nd, 2018

Providing strength and stability to the shoulder joint, the rotator cuff is surprisingly susceptible to injury. In fact, rotator cuff injuries are common among both the young and active, and older, more sedentary patients we see at Collins Place Physio. So, what exactly is the rotator cuff, what does it do, and how can you keep yours happy and healthy?
The rotator cuff is a group of four muscles and their tendons that arise from the shoulder blade and attach to the head of the humerus (upper arm), forming a cuff. It centres the humeral head in the shallow socket, and provides strength and stability during motion of the shoulder joint. It helps you to abduct (raise your arm to the side), and internally and externally rotate the shoulder.
Rotator cuff injuries are very common in people over the age of 40 due to normal age-related ‘wear and tear’ in the tendons. In younger patients, injuries are mainly due to a trauma to the shoulder, or overuse caused by repetitive overhead sports like tennis or volleyball. Rotator cuff injuries are also common in occupations that require working overhead or involve repetitive physical tasks, such as painting, carpentry etc.
Rotator cuff injuries usually start with a nagging ache in the shoulder when lifting/reaching overhead, dressing, or lying on the shoulder at night. This develops into pain and weakness with repetitive use, or when lifting the arm overhead.
As the shoulder joint is so mobile, it depends on the strength of the rotator cuff muscles and tendons to stabilise the joint. To prevent injuries to the shoulder, it is important to strengthen the rotator cuff as well as the bigger muscles around the joint.
Rotator cuff exercises should therefore be incorporated into all gym programs that involve upper body strengthening. You also need to strengthen the muscles that stabilise the scapula, as this provides the base for all shoulder movements. If one of these muscles is weak, it places more stress on the rotator cuff tendons at the front of the shoulder.
Thoracic (upper back) mobility is also essential in preventing rotator cuff tears and shoulder injuries. Poor mobility in the thoracic spine will cause a person to have reduced thoracic extension and rounded shoulders. This places a lot more load on the rotator cuff tendons and can increase the risk of injury.
Treatment will depend on the severity of the injury, and the patient’s lifestyle. Partial thickness tears will usually heal themselves with rest and the appropriate rotator cuff strengthening program. Full thickness tears, however, may need to be surgically repaired if the person is returning to high level sport or activity.
Older individuals can typically return to normal function through conservative management that involves strengthening the remaining muscles of the rotator cuff. Rehabilitation involves strengthening the rotator cuff, the muscles that stabilise the scapula, and working on improving general mobility.
If you are experiencing any shoulder pain or weakness, please call Collins Place Physio on 9650 2220 to discuss an appropriate rehab or prevention program.
Posted by Peter Hunt in General on October 29th, 2018

While a taut, toned backside might be on your wish list, having strong gluteal muscles is important for functional as well as aesthetic reasons. Comprising of a group of muscles in the buttocks – gluteus maximus, medius, and minimus – the glutes control external and internal rotation of the hip joint, extension and abduction of the leg, and help maintain pelvic stability during activities.
Strong glutes can improve your posture, balance, and sporting prowess, while reducing your risk of injury and back pain. With such an important role, they shouldn’t be neglected. So, read on to discover five common signs your glutes could benefit from some strengthening!
Unless you’re recovering from a squat-laden gym session, your glutes probably shouldn’t be feeling tight or sore. More often than not, chronic muscle tightness is a sign of weakness.
Posture isn’t only about a strong and stable core. Weak glutes can also cause an inability to maintain an upright posture through the trunk and pelvis.
If you suffer from hip or knee pain, you might be searching in the wrong place for the cause, as it is often glute-related. Weak glutes can cause strain on the hip itself, as well as the lower down joints of the knees and even the ankles.
If you’ve ever experienced lower back pain during bridging exercises at the gym or pilates, it’s highly likely you weren’t properly engaging your glute muscles. Weak glutes or glutes that aren’t ‘switched on’ can result in over-compensation from the lower back muscles. This can in turn cause pain and, potentially, injury.
Part of the glute plays an important role in keeping a stable pelvis during single leg activities, such as walking, climbing stairs, hopping or running. Lack of pelvic stability can cause strain above or below in the kinematic chain, for instance in the lumbar spine, knee or lower leg.
If you are experiencing any of the above concerns, please call us on 9650 2220 to make an appointment to have your gluteal function assessed, and a strengthening program prescribed.
Posted by Peter Hunt in General on October 24th, 2018

Pregnancy is a time of joy and excitement, but it can also take its toll on a woman’s body. At the same time, anxiety levels are often elevated, making stress management important. Regular massage can be particularly useful to alleviate this stress, while also having a host of other benefits. Read on to discover the many and varied reasons to include massage in your pregnancy self-care plan.
Hormones produced during pregnancy cause the pelvic ligaments to loosen and joints to open, which in turn places stress on weight bearing joints and structures. As a result, lower back pain is a common complaint during pregnancy. By increasing blood flow to muscle groups and allowing them to work more efficiently, massage can help to alleviate pregnancy-related back pain.
You’ve no doubt had a pregnant friend complain about their swollen ankles, or experienced it yourself. This is due to the fact a woman’s blood volume can increase as much as 40-60% during pregnancy, placing an additional load on the lymphatic system and increasing fluid retention.
Stimulating the soft tissue during massage will help to reduce the collection of fluid and assist the lymphatic system to effectively remove fluid. Hence reducing any swelling.
As the baby grows, some women may experience sciatica – characterised by sharp pain from the lower back down the back of the thigh and lower limb to the foot. Releasing the surrounding muscles and massaging the glutes and lower limbs can alleviate the pressure caused by the compression of the sciatic nerve.
Found on the palm-side of your wrist, the carpel tunnel houses several tendons and nerves that directly control your hands. Unfortunately, during pregnancy a large number of women will experience carpal tunnel syndrome due to excess fluid (oedema) in the wrists. As a result, they may experience pins and needles, numbness, and stiff, painful hands. Massage assists in moving the fluid and reducing muscular tenderness.
Hormonal changes during pregnancy can contribute to more frequent and intense migraines or headaches. By boosting circulation and reducing tension, massage can help relieve your pain.
Not only is massage very relaxing, it is known to promote a good night’s sleep. Magic words for any mum-to-be!
Posted by Peter Hunt in General on October 11th, 2018

While washboard abs might be out of reach for many, core strength is something we can, and should, all strive for. And its importance goes far beyond vanity and a flat stomach! A corset-like group of muscles that includes your rectus and transverse abdominals, pelvic floor, and obliques, the core muscles provide support and stability to your spine, both when you are static and moving.
Your core helps support your posture, protect your organs and central nervous system, and help you to stand, bend, lift and twist without injury. And that’s just for starters! Read on to discover six major benefits of building a stronger core.
Weak core muscles are a very common contributing factor to back pain. If you are not engaging your core, even while you are sitting at your desk all day, your lower back muscles will be recruited to keep your upright. The excess loading of these muscles will often lead to fatigue and unnecessary back pain.
A strong core automatically improves your posture by allowing you to sit and stand more efficiently, creating a feeling of increased stability and power. Instead of slouching and shrinking, you’ll sit and stand taller, making you instantly appear – and feel – more confident.
Good news for dieters – tightening this ‘corset’ of muscles and improving your posture will give you a slimmer silhouette and flatter stomach, regardless of the number on the scales.
A strong, stable core provides a good foundation for all of your movements. When the core is weak, your body will move less efficiently. Other parts of your body will pick up the slack and experience overloading, which can result in pain and injury.
With a stronger core, the body’s movement pattern is more controlled, requiring less energy to be spent compensating for poor movement patterns. A stronger core also allows your upper and lower limbs to work off a more solid base, allowing for increased force production. This enables the body to support/withstand greater loads in the gym, and produce more concise movement patterns on the sports field.
If you are experiencing bladder leakage, speak to your physio. A program to strengthen the deep pelvic floor muscles, particularly after childbirth, may be required. Exercises that engage the pelvic floor, such as yoga and Pilates, may also be beneficial.

Whether you’re a Pilates devotee or brand new to the practice, you’ll gain a lot from Pilates classes at The Alignment …

If we’ve seemed distracted the past few months, it’s because we’ve been working on a little something that’s actually kind …

Maintaining healthy, happy feet is extremely important—after all, you’re on them for much of the day! Without foot comfort, your …